As a health care professional, it’s important for you to establish good communication and trust...
VIEW ALL

Developing Good Rapport With Patients

“I’m Sorry” Laws and Lawsuit Risk
Miscommunication or poor communication between health care providers and patients or their fami...

Organizational Strategies to Reduce Work Stress for Health Care Professionals
Work stress is an unfortunate reality of much of the health care industry. The National Institu...

Reducing Laboratory Errors
Lab testing forms the basis for many aspects of diagnosis and treatment. This means that test-r...

Medical Liability Terminology That Health Care Professionals Should Know
You probably learned basic legal terminology while you were getting your degree and other train...

Communication is Key for Patient Care
According to the Institute for Healthcare Communication, “Extensive research has shown that no ...
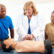
Liability Concerns for Health and Safety Educators
As an educator specializing in health and safety education, you have the satisfaction of knowin...

The Impact of Nursing Workloads on Patients
Study after study has shown that nurses around the world are burdened with heavy workloads. Thi...


